By Leo John
From Processing to Documentation, it is difficult for the healthcare administrators to focus on main operations. To reduce the administrative burden, Revenue Cycle Management is used to authorize the patient’s information and ensure a decrease in claim denial. To reduce errors and increase the company’s revenue and build trust among patients, RCM service is being utilized.
Benefits of Outsourcing RCM
Many hospitals suffer from inefficient workflows, staff insufficiency and errors.Outsourcing Revenue Cycle Management Solutions to an experienced company enables them to overcome problems and raise financial performance. Customizing RCM helps to build trust between hospitals and patients.
1. Improves Efficiency and Revenue
Outsourcing helps you to simplify Billing and Coding processes, reduce claim denials, and ensure timely compensations. Proficient vendors use advanced technologies and best methods to optimize RCM workflow. You can see benefits such as reduced errors in Coding and Billing and decrease in denials.
In hospitals, RCM services enhance efficiency, allowing staff to focus on patient care and other main activities. The outsource company handles the RCM staff and supervises the regulatory issues. Registration, Insurance Authentication, Eligibility Validation and Patient Information are managed by outsourced staff.
2. Expertise Access and Technology
Leading RCM companies have access to trending technologies and innovations such as Artificial Intelligence, Machine Learning, Automation and Cloud Computing. Vendors must integrate surviving platforms such as Billing Software and other systems for RCM.
3. Data Privacy and Security
Hospitals ensure the vendors follow the necessary rules and regulations and they have adequate safeguard measures for Data Protection and Data Availability. Hospitals need to monitor and validate RCM vendors and have possibility plans in other incidents. If you provide access to vendors to handle financial data for sensitive patient, it may include security and other risks. Research and ensure that the company you prefer to handle your Revenue Management maintains loyalty and reputation to protect data.
Increase in profit gaining and removing unnecessary administration burden enables you to focus on patient services. While medical staff take care of patient healing, RCM services enable administrators to enhance financial performance. To attain maximum advantages from RCM, administrators must have a keen focus on resources such as coding, privacy, and security.

Financial Benefits of RCM Services
The scope of RCM services does not only focus on Billing and Coding, but enables accurate, quick billing and enhances potential revenue. Hiring costs and training costs increase, pending of claims and denials rate significantly decrease when administrators track the process. Research has reported that additional payments are going down with RCM Services.
Key Factors for Usage of RCM Services

- Simplifies Workflow Process
- Increases Medical Diagnosis Identification
- Decreases Backlogs and Errors
- Improves Documentation
- Enables Information and Financial Performances
Potential Challenges we Face in RCM
Partner with an experienced RCM company that focuses on minimizing challenges such as:
Communication Delay
Communication space may affect Productivity, with different systems as a factor. These affect the quality of services such as Billing and Coding.
Conflict Between Agents
There may be differences in goals and incentives of vendors and hospitals. Vendors prioritize gaining profits. This conflict-of-interest damages the relationship between hospital and vendor.
Why is RCM Important for Patients and Healthcare Service Providers?
Do you know why Revenue Cycle Management is considered important? The ultimate goal of RCM in raising the company’s revenue benefits the patient more than anyone else. You can see the decrease in time spent on administrative and clinical tasks. This ensures you that more time is spent on patient care and their treatment. We are established, experienced, dedicated and available to help you with several healthcare facilities that enable best patient care.
Our Revenue Cycle Management Workflow
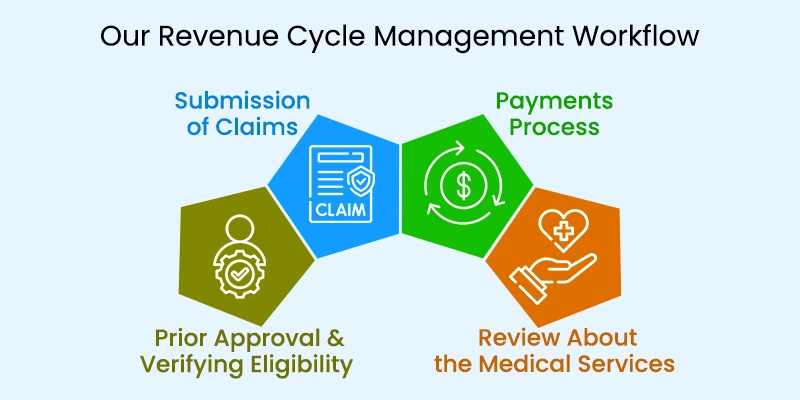
RCM service is performed by including several steps. You must notice that it determines that there are many possibilities for error occurrence. Any error in the revenue cycle can delay the Revenue Cycle Management Healthcare service provider’s compensation from patients or insurers. To have a better understanding of where errors occur and how RCM prevents them, look into the steps involved in Revenue Cycle Management.
i) Prior Approval and Verifying Eligibility
When a patient makes an appointment, the provider maintains the patient’s account and collects information. This involves collecting the patient’s insurance details and validating the patients’ insurance eligibility.
RCM justifies the validation status, even if a patient has an account with the provider previously. Claims of the patient with inaccurate information and ineligible assurance status will be denied. It also leads to delays in payment compensation. This gives more burden for the provider to check the patient’s information and correct the errors made.
Medical services are being reproduced into charges using codes that are universally accepted. This code determines how health insurance companies decide. If the Medical Coding is not proper, the patient’s claim is being denied by the insurance company. This also may cause a delay in payment. However, these denied claims would have also included verification process. The Revenue Cycle Management process involves a verification process to track claim denials. Effective RCM ensures entering correct medical codes to avoid claim denials.
ii) Submission of Claims
When a patient’s medical service is correctly coded, the claim is moved to the insurance company for approval. RCM makes sure that the claim submission processes quicken the tracking and claim management from the start of the process.
iii) Payments Process
After the approval of the patient’s claim, the insurance company repays the provider based on the patient’s eligibility. If there is any balance remaining, then the provider’s reach the patients and collect payments.
Revenue Cycle Management facilitates the Medical Billing process by simplifying the claims. Since the RCM focuses on insurance eligibility and validation, the patients will know about their payment status at the beginning. This helps in avoiding payment delays.
iv) Review About the Medical Services
Revenue Cycle Management supports healthcare providers to research about clinical data. This data analysis enables healthcare providers to identify where the errors occur and how to reduce the possibility of errors. This in turn increases the revenue and improves patient experience.
Benefits of Healthcare Revenue Cycle Management
Revenue Cycle Management process supports providers to avoid delay or loss of revenue. In addition to enhancing the provider’s revenue RCM serves several benefits. These benefits not only help providers but also patients and this adds the value of Revenue Cycle Management process even greater. Let’s see the benefits of RCM:
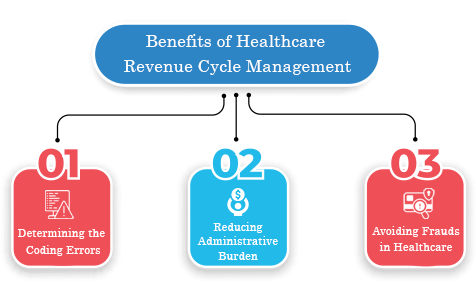
1) Determining the Coding Errors
By enabling the RCM execution, providers can easily recognize the point of error occurrence in the Medical Billing process. This helps to predict the occurrence of future claim denials. Analysis suggested that more than 90% of denials are due to issues such as lack of details, or improper coding. If these errors do not occur and claim approval is done after first submission, providers receive their payments quickly. So, there is no necessity to spend additional costs to enquire and request for denied claims.
ii) Reducing Administrative Burden
A minimal administrative burden can be achieved with the prevention of claim denials. If there is no need for administrative staff to spend time on enquiring and requesting denied claims, more time and energy will be available to spend it on efficient patient care. Also, RCM focusses on simplified interactivity between patients and staff. Scheduling appointments, Form completion, Claim submissions and Medical billing process is smoothened to provide efficient and satisfactory experience for all.
iii) Avoiding Frauds in Healthcare
The significant benefit of RCM service is the protection from fraud. Healthcare fraud fetches billions in healthcare every day. Fraud validation affects the revenue and reputation of a healthcare provider.
These types of fraud investigations are caused due to inaccurate Medical Billing. Some common issues in Billing code include services are not being provided, unwanted medical procedures, services performed by unqualified employees, and low-quality procedures. Providers also include procedures such as requesting a higher payment rate for services.
With Revenue Cycle Management importance on data collection, Medical coding, there is less chance of providers submitting inaccurate data. RCM gives all the updated rules and regulations.
How to Avoid Fraud Patients?
Patient fake information may also be a source of healthcare fraud. It takes in two ways:
Inaccurate Information
Some patients may provide false information to receive unqualified services. Administrative staff will track inaccurate insurance coverage.
Capturing Medical Theft
Today, in the healthcare industry, medical theft has been a rising concern. RCM begins with validating patient’s information, so any identity theft that occurs will be identified at the starting stage of the process.
Conclusion
MHRCM has provided you with many insights in this blog. The suggested discussions enable you to understand how RCM services improve revenue and reduce administrative burdens. By avoiding errors, claim denials, and fraud investigations, healthcare providers enable efficient reimbursements for their services. Also, the Revenue Cycle Management enables providers to avoid spending more time for claim requests, solving errors, and fraud investigation. With more revenue, providers can invest more in patient care, because patient care is the top priority for any Healthcare Provider.
Frequently Asked Questions:
What Are The Benefits Of Healthcare RCM?
Healthcare RCM combines administrative information such as patient identity, insurance plan, and patient demographics to the healthcare that a patient receives. It helps you save time and money by reducing the denied claims and enabling the possibilities of patients to make online payments.
How Important Is RCM In Increasing The Revenue?
Revenue Cycle Management plays an important role in maximizing revenue. By researching and analyzing, Revenue Cycle Management enables businesses to optimize pricing and gain more profits.
What Are The Strategies That Help To Control The Revenue?
There are many strategies involved that help to monitor and control revenue such as analyzing the market, collecting the user needs, choosing the best rate, focusing on customer retention and mobile optimization, and adding Revenue Management tools.
What Is Meant By Revenue Cycle?
A Revenue Lifecycle is the set of activities a customer experiences starting from engagement to purchase and beyond that. Understanding customers’ move throughout the process enhances the revenue.
What Is Meant By The Revenue Cycle Coding?
Revenue Cycle Management includes coding that facilitates managing administrative tasks such as Patient registration, Verification, coding, Claims processing, Data collection and all other aspects of revenue generation.
Related Resource :
About the Author





