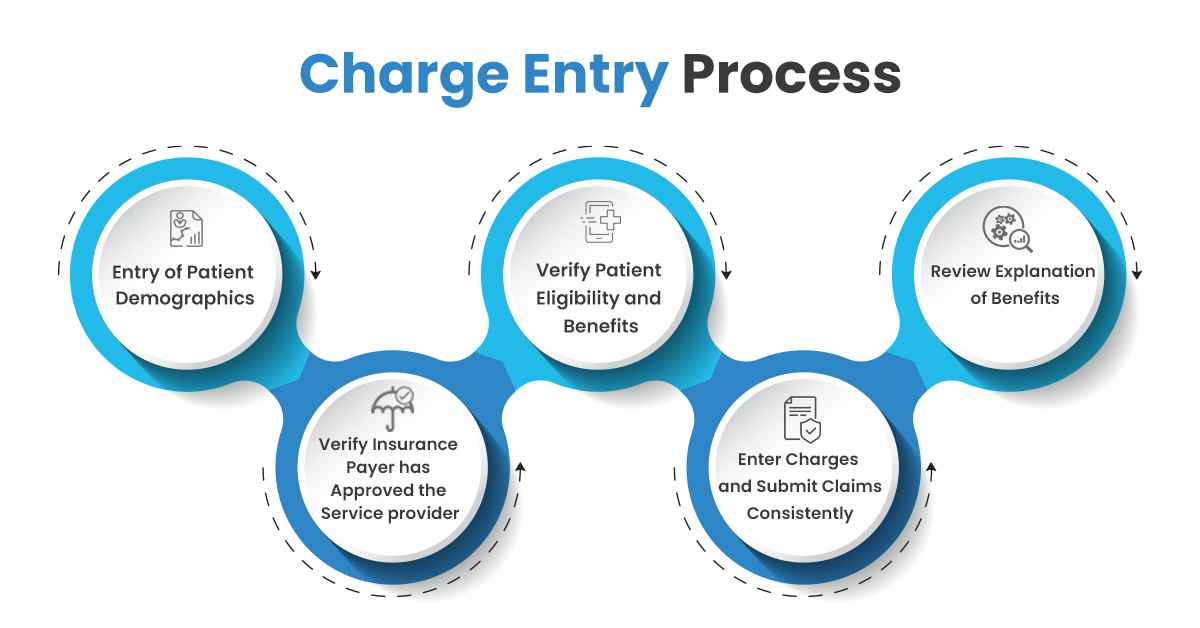
Charge entry is the process by which charges for a medical procedure and patient’s facing practices are collected and submitted to the appropriate payors for billing. Moreover, charge entry involves detailed accounting for service rendered and the initial intake of important information.
The data that needs to be collected for entry begins with patient information, demographic, insurance details or payment options and health history. Along with that, there is more information collected about payors as well as details of medical care appointments (date, care provider who attended, services provided etc.)
As noted above, charge entry is a substantially more extensive Medical billing . An accurate and seamless record-keeping is essential to get maximum reimbursements. Even an individual error in a reported charge can lead to minor miscommunication and still set for more impactful errors down the road. While we look at eliminating errors, charge capture is crucial to managing denials and a path toward profitable revenue payments.
The majority of claim denials are due to administrative errors. To avoid the room for claim denials, accurate patient demographic submission is indispensable. Ensure the patient and guarantor’s name, ID, date of birth, age, gender, address, phone number, and most importantly, insurance details.
Foremost, ensure you include all the following details on your superbill before proceeding with your in-house clearing department or third-party payors. Besides, you should pay attention to some of the significant entries during the charge entry process. It includes the date of service, place of service, date of admission, pre-authorization details, rendering provider details, and modifiers (if needed).
It’s crucial to submit and track healthcare service provider credentialing and re-credentialing applications based on the insurance plan. Provider credentialing is the process of collecting and authenticating a healthcare provider’s credentials. That validates that the provider has the necessary license, certification, and skills to care for a patient.
Patient eligibility verification is one of the best ways to maintain clean and clear claims. However, the eligibility verification process is often neglected by some healthcare organizations. The eligibility verification in the charge entry medical billing process is critical before submitting insurance to the in-house clearing team or third-party payors. Because eligibility verification ensures the insurance data is appropriate and helps determine the amount that the patient may need to owe. Also, providing an accurate cost estimate can boost patient satisfaction.
Make your team available to enter charges during the charge entry process without delaying the entry. Also, post charges the same day the patient provides the service. Because the longer you take to post charges, the longer it takes to file a medical claim.
The explanation of benefits (EOB) is the statement the insurance company sends after processing a claim submission from the healthcare provider. The EOB statement contains the total charges, non-covered amount, allowed amount, and amount paid to be the healthcare provider, patient deductibles pay.
By analyzing the EOB, you can gather and determine that you need to perform a more in-depth investigation and what further actions are required.
With the seamless charge entry, services or practices rendered by the healthcare professionals are transcripts into the codes. Each service is accurately charged to obtain the proper and faster reimbursements.
Prevent Claim Denials and Rejections
Regular data entry consumes more administrative function time and effort for identifying errors. It could take weeks or months to find and solve the errors if any occur. However, the charge entry can change the process. Systematic charges entry in revenue cycle management companies will help reduce investigating costs.
Having specialists in the medical billing team for the charge entry can benefit healthcare centers by making the revenue cycle function better. With the charge entry specialist, you can take notes of patient information daily and update them according to the latest documents. Moreover, revenue cycle management in healthcare needs to be attentive to several components of the billing team. The professional makes it a point to inform decisions with every sub-departmental.
There is no doubt that the flawless revenue cycle needs accuracy in each administrative and clinical follow-up process. Get in touch with the expert Medical billing to increase charge entry and bill accuracy with proper diagnosis codes and procedural codes in a vital revenue cycle process to ensure that the claims don’t face denials. Streamline your administrative process by outsourcing charge entry and medical billing with MHRCM from eligibility verification to charge entry, from billing & coding to claim follow-ups.