Revenue Cycle Management is necessary for managing a successful medical practice. It will directly affect your bottom line. More significantly, Revenue Cycle Management Strategy directly impacts the patient and their experience. Revenue Cycle Management (RCM) stands at the forefront of organizational success. The efficient Revenue Cycle Management Process is not a financial endeavor but a strategic imperative that directly impacts a Healthcare Institution’s ability to thrive and provide optimal services.
Why is Revenue Cycle Management Important?
The Medical Revenue Cycle consists of many steps, all of which are crucial to ensuring prompt provider repayment. Because they require accuracy, tasks like account creation, pre-registration, insurance eligibility verification, claim processing, and medical coding take more time to complete. But in order to receive reimbursement quickly, these chores also require speed. That’s why you’ll need to make adjustments and improvements where you can.
The Fundamentals of Solid Revenue Cycle Management
Eligibility verification is the essential first step. When a Medical Revenue Cycle provider confirms a patient has active health insurance, the provider can bill rather than pursue full payment from the patient. It is ideal for the provider because patients usually don’t have the means to pay their bills in full out of pocket, but health plans do.
Finally, if a claim is denied, billers can edit the claim to correct mistakes and re-file it for payment. It is referred to as denial management in the Revenue Cycle Management Process.
However, as brief as eligibility verification, claims submission, and denial management may sound, many challenges can come up throughout the process, and additional steps providers can take to improve their Revenue Cycle Management Healthcare success.
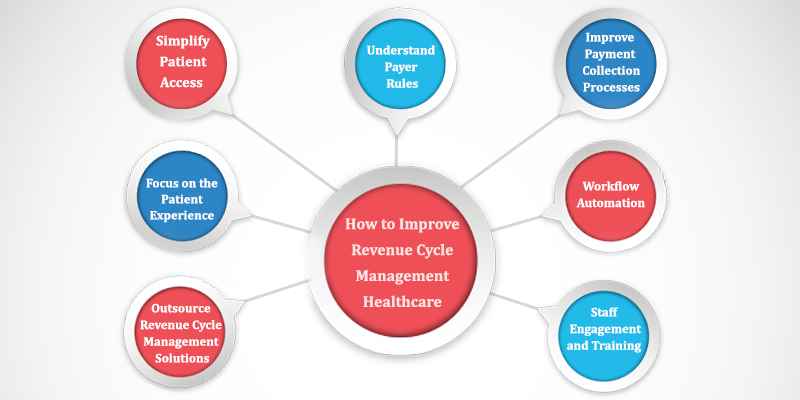
How to Improve Revenue Cycle Management Healthcare
The best way to improve Revenue Cycle Management Healthcare is to break the process down into multiple components and then focus on making each step as efficient as possible. Consider everything from the very first patient interchange to the final payment, and think about staff engagement and billing aids, too.
Patient access is the entire new patient process. Eligibility verification is part of it, but this is not the only step. Revenue Cycle Management Process Patient Access also includes verifying patient demographics such as first and last name, current address, and Social Security Number. Additionally, Medical Revenue Cycle Management providers should verify any coverage beyond what the patient has provided for confirmation.
It’s common for patients to have secondary coverage that they are either unaware of or have not disclosed. It doesn’t have to create more work for front-of-house teams. Managing all the details of patient access is easy with the right software to store patient data and get ahead of potential downstream Revenue Cycle Management mistakes.
Regarding potential Medical Revenue Cycle mistakes, let’s consider payer rules. Medicare and commercial payers have rules regarding what codes to use and how to submit claims. And those Medical Revenue Cycle payers’ rules can change at any moment. For many Medical Revenue Cycle billers, keeping up with all the changes to those rules can feel like a second job, particularly for those in large provider organizations that work with multiple Medical Revenue Cycle payers. For those equipped with a claims submission tool that figures out payer rules on their behalf, ensuring every claim is sent to the proper payer and adhering to the latest Revenue Cycle Management Solutions is much easier.
Improve Payment Collection Processes
While it’s great to know Medical Revenue Cycle claims are submitted to payers correctly, the patient commitment may be their co-pay with coverage, or they may not have active coverage to compensate for their balance. Either way, it’s up to Revenue Cycle Management Solutions billing teams to capture patient payments.
Another common way to improve the Revenue Cycle Management Process is through workflow automation. This can be done during patient access, claims submission and payment collection processes, denial management, and more. To automate patient access in Revenue Cycle Management Services, implement a coverage discovery tool that can search for all active Medical Revenue Cycle payers at once and replace the need for individual payer inquiries. During claims submission and denial management, workflow rules like grouping claims by type of payer or assigning them to a precise biller can turn a digital “pile” of thousands of claims into a systematized set of claims for each person to focus on.
Staff Engagement and Training
Every front-office and back-office person plays a crucial role in improving the Revenue Cycle Management Process. Staff engagement begins with making each person’s value clear and then providing them with the tools they need to succeed. For each newly automated workflow, multiple opportunities are provided to train and get acquainted with the updated processes. Make training a priority for new billers, team managers, office administrators, and any other staff involved in the claim lifecycle.
Outsource Revenue Cycle Management Solutions
Of course, one of the easiest ways to improve your Revenue Cycle Management Services is simply to entrust them to an expert. Partnering with an expert is easy and efficient and removes the burden of revenue from your plate entirely. The Revenue Cycle Management Solutions manager will look for ways to improve your process efficiency to capture charges and get you paid faster.
Focus on the Patient Experience
Finally, it’s important to remember that the patient comes first, even in Revenue Cycle Management Strategy. Many steps throughout the Revenue Cycle Management Process can positively or negatively impact the patient’s experience. Allow new patients to provide their details via an online patient portal before their visit. It allows them the flexibility to offer necessary information for treatment on their own time and saves time during their appointment.
Improve Revenue Cycle Management Solutions with MHRCM